Hemostasis is a complex physiological process involving cells (platelets, especially but also fibroblasts), and soluble (coagulation factors and inhibitors) and insoluble proteins (extracellular matrix proteins). The hemostatic system is usually activated upon injury to the blood vessels, which disrupts endothelial cells exposing thrombogenic (or procoagulant) substances in the extravascular space. Once activated, the hemostatic system serves to seal off the injury through platelet plug and fibrin clot formation. This allows time for the injured endothelium to heal. Once healed, the clot must be dissolved (fibrinolysis) to restore blood flow.
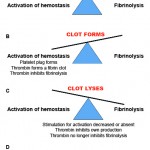
The hemostatic system is really a delicate balance of pro- and anticoagulant forces and can be thought of a pendulum that swings between these forces. Initially on vessel injury, procoagulant forces dominate resulting in a fibrin/platelet clot, which seals off the injured blood vessel. Once the endothelium has healed, the pendulum swings in favor of anticoagulant and profibrinolytic forces, allowing clot lysis and restoring blood vessel patency.
Alterations in this delicate balance can result in hemostatic abnormalities, which can manifest as either hemorrhage or thrombosis. Most animals with hemostatic disorders present with clinical signs of excessive hemorrhage. In contrast, thrombosis is far more difficult to detect clinically or by laboratory tests, particularly when it occurs in internal microvessels. When any animal presents with clinical signs of a hemostatic disorder (hemorrhage or thrombosis), it is essential to do a complete diagnostic evaluation, including performing a thorough physical examination and taking a detailed history. Vital clues as to the underlying cause of the hemostatic disorder are obtained from the signalment (age, breed and sex), history (e.g. access to toxins or drugs, evidence of multiple hemorrhagic episodes) and clinical signs (e.g. type and location of hemorrhage).
This section is organized as follows
- Physiology: Information on how hemostasis works, distinguishing processes of primary hemostasis, secondary hemostasis, fibrinolysis and inhibitors.
- Diagnostic approach: How to work up a patient with a hemostatic disorder.
- Clinical signs: Expected clinical signs associated with hemostatic disorders.
- Sample collection: Crucial!! How not to mess up hemostatic test results, which are majorly affected by preanalytic (sample collection and storage) variables.
- Tests: Different tests of hemostasis, separated into sections based on
- Primary hemostasis: Platelet number and function, buccal mucosal bleeding time (BMBT), von Willebrand factor (vWf).
- Secondary hemostasis: Screening assays, fibrinogen.
- Fibrinolysis
- Inhibitors, including therapeutic heparin monitoring.
- Global tests: Viscoelastic testing (e.g. thromboelastography, thromboelastometry).
- Diagnostic algorithm on screening test interpretation
- Quick table summaries on mechanisms of thrombocytopenia and coagulation screening test result interpretation.
- Disorders: Disorders affecting hemostasis.
- Test summary: Table summarizing changes in hemostasis test results with various disorders.
- Primary hemostasis: Vessel wall defects, thrombocytopenia, thrombopathia, von Willebrand disease.
- Secondary hemostasis: Inherited factor deficiencies, vitamin K deficiency/antagonism
- Inhibitors
- Global disorders: Disseminated intravascular coagulation, underlying disease, drugs.
- Transfusion medicine
- Blood collection for transfusion purposes.
- Blood components used for transfusion, e.g. whole blood, packed red blood cells, cryoprecipitate.
- Blood types: The different blood groups in animals.
- Cross-matching: How and when this test is performed.
- Transfusion therapy: What and how to administer transfusions, with dose guidelines.
- Adverse reactions: Immune and non-immune mediated reactions to transfusions.
