Interferences are substances such as lipids, free hemoglobin and bilirubin (also globulins and drugs) which affect the results of clinical pathologic tests, as they are being performed. They are considered analytical variables because they directly interfere with test performance (and results) in various ways, but also are pre analytical variables, because some (lipids, free hemoglobin, drugs) are controllable to some extent and can be minimized by sample collection and handling. In this section, we will cover the effect of the three most common interferences in clinical pathologic testing, lipemia, hemolysis and icterus. There is also a quick summary of potential effects of these interferences on hematologic and clinical chemistry test results. The effect of these variables on clinical pathologic testing is method dependent and also dependent in the degree of change (for all testing, including hemostasis). See individual test results for more details on how these interferences affect results, with methods used at Cornell University. With our chemistry analyzer, we also provide guidelines as to how these preanalytical variables affect our results. Of these interferences, hemolysis is the most common (mostly collection-associated or preanalytical, but can be due to an intravascular hemolytic anemia) (Whipple et al 2020).
Lipemia

Lipemia (lactescence) is caused by increased triglycerides (usually as chylomicrons and, infrequently, from high concentrations of very low density lipoproteins). Lipemia is usually a post-prandial artifact (blood collected in a non-fasted animal) and can be minimized by collecting blood from a fasted animal (minimum, 12 hour fast). In fact, lipemia in a fasted animal usually indicates the presence of an underlying disease involving metabolism, e.g. diabetes mellitus, pancreatitis, hepatic lipidosis (horses), neoplasia (thoroughbreds).
Hematology testing interference
Lipemia interferes with hematology tests by the following mechanism by light scattering. This affects the following results:
- Hemoglobin and hemoglobin-related indices: Results in falsely increased absorbance readings of hemoglobin, causing a falsely high measurement. This will manifest as a high mean cell hemoglobin (MCH) and mean cell hemoglobin concentration (MCHC) so these results are often cancelled. This interference is largely overcome with the hematology analyzer at Cornell Univesrity, which directly measures the hemoglobin content in RBC (corpuscular hemoglobin, CH and corpuscular hemoglobin concentration, CHCM) by laser light scatter. In lipemic samples, we generally report these values from the analyzer (calculated hemoglobin, CH, CHCM) when lipemia falsely increases the standard hemoglobin (MCH, MCHC) measurement.
- Total protein by refractometer: Large lipids like chylomicrons refract light, falsely increasing total protein measurement with this technique.
- Platelet count: In severe lipemia, large lipid molecules may be counted by the analyzer erroneously as platelets, falsely increasing the platelet count.
Chemistry testing interference
Lipemia interferes with chemistry tests by the following mechanisms (but the effect is dependent on the degree of lipemia; see rough guide):
- Light scattering: Results in falsely increased absorbance readings of some analytes, particularly those that are endpoint reactions that are not blanked, e.g. total bilirubin, resulting in high concentrations of bilirubin. This is method dependent (lipemia minimally affects bilirubin results from the analyzer used at Cornell University).
- Volume displacement/solvent exclusion: This falsely decreases values of some analytes, e.g. electrolytes (mostly sodium and chloride, which are decreased proportionately, but also potassium to a lesser extent).
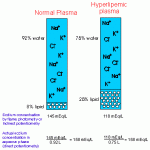
Volume displacement of chemical constituents by large particles (lipid, protein) - Hemolysis: Hemolysis of erythrocytes is enhanced in the presence of lipemia. This can affect results of individual tests (particularly end point reactions that are not blanked), because hemoglobin will absorb at wavelengths used to detect reactions in the analyzer.
At Cornell University, we generally try to minimize artifactual changes in laboratory results from lipemia. This is done by refrigerating and centrifuging the plasma/serum at high-speed, which forms a fat layer at the top of the sample. The less lipemic plasma below the fat layer is aspirated from the tube and used for analysis. Chemical clearing methods are unreliable and may affect laboratory results in other ways, so they are generally not used to clear lipemic plasma. Note that triglyceride measurements must be performed on un-adulterated samples, because otherwise values will be falsely decreased if the fat layer is not included in the analysis. See individual test results for more details on how lipemia interferes with results, with the methods used at Cornell University.
Hemolysis
Hemolysis is usually an in vitro artifact due to poor venipuncture technique, lipemia, freezing of whole blood samples, delayed separation of serum or plasma from cells, delayed sample submission, and certain anticoagulants (fluoride-oxalate). Red blood cells are also more fragile in lipemic samples and tend to lyse more readily in these samples, even if the blood is stored or handled correctly. However, hemolysis can occur in vivo when there is intravascular hemolysis with certain types of hemolytic anemias (e.g. Babesia infection, oxidant injury). Artifactual RBC lysis can mimic intravascular hemolysis and it can be very difficult to distinguish in vitro from in vivo intravascular hemolysis (particularly in the laboratory where all we see is the sample and not the patient). However, if the animal is anemic and has hemoglobinuria, true in vivo intravascular hemolysis, i.e. a pathological hemolytic anemia, is likely. in the past, when hemoglobin-based oxygen carriers (such as Oxyglobin) were available, they would interfere substantially with results obtained from hematology and chemistry analyzers (For more information on HBOCs, see controllable pre-analytical variables), however these products are no longer used.
Hematology testing interference
Hemolysis (in vitro or in vivo intravascular) interferes with hematology tests by the following mechanism by lysing RBC and light scattering. This affects the following results (but the effect is dependent on the degree of hemolysis; see rough guide):
- Hematocrit (HCT), packed cell volume (PCV) and RBC count: With in vitro hemolysis, these results will be falsely low because the lysed RBC are not included in the count or measurement of the PCV (remember the HCT is a calculated result, dependent on the MCV and RBC count, which are measured directly by the analyzer). With in vivo intravascular hemolysis, these results reflect the intact red blood cells available to carry oxygen (true measure of oxygen carrying capacity).
- Hemoglobin-related indices: Because automated analyzers deliberately lyse RBC to measure hemoglobin, the hemoglobin measurement is the same with or without hemolysis (in vitro or in vivo intravascular). With in vitro hemolysis (artifactual), the hemoglobin is the most accurate measure of the animal’s oxygen-carrying capacity and a HCT can be estimated by multiplying the hemoglobin x 3 (since hemoglobin usually comprises 1/3 of the red blood cell). With true in vivo intravascular hemolysis, the HCT, RBC count or PCV are a more accurate measurement of the oxygen-carrying capacity of the animal, because the lysed RBC and free hemoglobin cannot carry oxygen. Regardless, in vitro or in vivo intravascular hemolysis results in a higher hemoglobin result relative to the HCT and RBC count and indices related to these measurements, the mean cell hemoglobin (MCH) and mean cell hemoglobin concentration (MCHC) will be falsely high and may be cancelled. The mean cell volume (MCV) is directly measured by automated analyzers and is unaffected by these types of hemolysis (unless it is a calculated value from the PCV).
- Total protein by refractometer: In vitro or in vivo intravascular hemolysis blurs the line in the refractometer, making it difficult to read. Hemoglobin, as a protein, may also contribute somewhat to the refractive index measurement.
- Platelet count: In in vitro or in vivo intravascular hemolysis, ghost RBCs may be counted by the analyzer erroneously as platelets, falsely increasing the platelet count and the mean platelet volume.
Chemistry testing interference
Hemolysis (in vitro or in vivo intravascular) interferes with chemistry tests by the following mechanisms:
- Increased absorbance: Released hemoglobin increases absorbance in the hemoglobin spectral range. Many of the chemical reactions are based on measuring a change in absorbance around the optical density of hemoglobin. This can be offset by using kinetic reactions (which measure the rate of change in absorbance) or blanked endpoint reactions (which are the most affected by hemolysis).
- Inhibition of reactions: Released hemoglobin can directly inhibit chemical reactions.
- Release of intracellular constituents that are directly measured: Release of constituents or enzymes found in high concentrations in red blood cells will falsely increasing the results of these tests, e.g. potassium (which is high in horses, camelids, some breeds of cattle, and Asian dog breeds, such as Akita, Shiba Inu), AST, LDH, magnesium, and potentially iron (although iron is in the heme ring within hemoglobin, heme iron should not react with the reagent in the iron assay – in internal studies we have not observed a direct correlation between hemolysis and iron values in several domestic species). Note that phosphate can increase with in vitro or in vivo intravascular hemolysis with storage of the sample as organic phosphates are converted to inorganic phosphates over time.
- Release of membrane or intracellular constituents that participate in reactions: Release of enzymes which participate in chemical reactions, e.g. adenylate kinase or glucose-6-phosphate will increase serum creatine kinase (CK) activity because they participate in the reaction (are not directly measured).
- Water release: Release of red blood cell water can dilute serum constituents.
The effect of in vitro or in vivo intravascular hemolysis on test results is species-dependent (and dependent on degree as stated above).
- Swine: Di Martino et al 2015 generated hemolysis in porcine (Landrace x Large White pigs) RBCs by agitation and found that this had the following effects on serum analytes run on the Cobas 501 autoanalyzer:
- Mild hemolysis (correlating to a hemoglobin concentration of 36 mg/dL or <50 hemolytic index units) mildly decreased glucose (median decrease of around 7%, hexokinase method) and increased potassium (median, 1.3 mEq/L), phosphate (median 5% increase), magnesium (median, 6%), AST (median change, 10 U/L), GGT (median change, 9 U/L, Szasz method), total bilirubin (median, 47%), LDH (median change, 69 U/L) and uric acid (median change, 50%, uricase method).
- Moderate hemolysis (correlating to a hemoglobin concentration of 72 mg/dL or <100 hemolytic index units) led to further decreases in glucose (median, 10%) and increases in potassium (median, 1.9 mEq/L), phosphate (median, 9%), magnesium (median, 10%), AST (median, 20 U/L), ALT (median, 4 U/L), ALP (median, 7 U/L), GGT (median, 24 U/L), total bilirubin (median, 250%), LDH (median, 124 U/L), and uric acid (median, 100%).
- More severe hemolysis (correlated to a hemoglobin concentration of 127 mg/dL or >100 hemolytic index) decreased glucose (median, 14%), urea nitrogen (median, 10%, urease method), creatinine (median, 10%, enzymatic method), and cholesterol (median, 10%, CHOD-PAP method) and increased phosphate (median, 20%), magnesium (median, 10%), AST (median, 34 U/L), ALT (median, 7 U/L), ALP (median, 14 U/L), GGT (median, 60 U/L), total bilirubin (median 650%), LDH (median 220 U/L), iron (median, 15%) and uric acid (median, 200%). Potassium was markedly affected (not measurable).
- NEFA and lipase were also increased by hemolysis (however Cornell uses different methods for both these analytes).
- Haptoglobin and C-reactive protein (CRP) were increased by moderate to severe hemolysis, as defined in this study.
- Changes were attributed to the following:
- Analytical interference: CRP, haptoglobin, creatinine, cholesterol, GGT, NEFA, total bilirubin, iron, lipase, ALP.
- Cellular release: Potassium, phosphate, magnesium, urea, ALT, AST, LDH, uric acid.
- Dilution: Glucose, sodium (mild decrease), albumin (mild decrease).
Electrophoresis interference
Hemoglobin can migrate in the early beta region of the tracing, resulting in increased beta globulin fractions. The hemoglobin-haptoglobin complex can also migrate in this area. If the hemolysis is severe, a tall almost monoclonal-like spike may be seen in this fraction (with a somewhat broad base), that may be misinterpreted as a monoclonal immunoglobulin.
Icterus
Icterus has minimal to no effect on hematologic results, including plasma protein measured by refractometry (Gupta & Stockham 2014).
Chemistry testing interference
Bilirubin interference arises from its spectral properties and its ability to react chemically with other reagents (resulting in decreased analyte values). This particularly affects creatinine and total protein concentrations (Gupta & Stockham 2014), both of which are decreased with high bilirubin concentrations (>15 and >10 mg/dL total bilirubin, respectively). The effect is dependent on the degree of icterus; see rough guide.
Heinz bodies
In cats with diseases such as diabetic ketoacidosis, onion poisoning and lymphoma, large numbers of Heinz bodies (>50% of 1000 RBCs) may interfere with spectrophotometric measurements of hemoglobin, falsely increasing the hemoglobin (HgB) concentration in relation to the red blood cell (RBC) count and hematocrit (Hct), leading to falsely increased MCH (= HgB/RBC) and MCHC (=HgB/HCT). With ADVIA-based hematology analyzers, the default WBC count from the analyzer (from the basophil channel) can be falsely increased in rare cases (Dondi et al 2019, Johnson et al 2020). In two cats with many large Heinz bodies, the ADVIA had difficulty discriminating reticulocytes from mature RBCs, leading to a falsely decreased reticulocyte % and absolute reticulocyte count (Johnson et al 2020). With the Sysmex XT-2000iV analyzer, large numbers of large Heinz bodies in one cat was associated with a mildly falsely increased WBC count and a population of events between the RBC and platelet events on the optical cell volume by fluorescent (with an RNA-binding dye, polymethine) platelet cytogram (platelet-O), which falsely increased the reticulocyte count (% and absolute) and platelet count (Johnson et al 2020).
