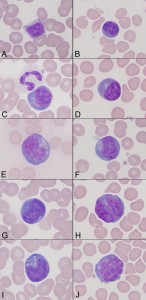
Reactive lymphocytes are seen in peripheral blood as a response to antigenic stimulation. Thus, they are more frequently in younger animals, who are antigenically naive. Any disease process can induce antigenic stimulation and result in the presence of reactive lymphocytes in circulation, thus it is a relatively non-specific finding. Reactive lymphocytes are heterogeneous – they vary in size and morphologic features (nuclear shape, amount and color of cytoplasm). They all have relatively mature clumped nuclear chromatin and no visible nucleoli. Their nuclear shapes vary quite markedly. Some have increased amounts of deep blue cytoplasm with perinuclear clear zones (representing the Golgi) and resemble plasma cells. This heterogeneity in size, shape and appearance is most compatible with a reactive lymphoid population.
Since some reactive lymphocytes can be quite large and slightly unusual in appearance (see E to J in the image to the right), it is of paramount importance to distinguish reactive lymphocytes from neoplastic hematopoietic cells. This is best done by an experienced clinical pathologist, who uses a variety of information (signalment, clinical signs, morphologic features of the cells in question), to make a distinction between reactive lymphocytes and neoplastic cells. However, this is not always possible and when cells that cannot be readily identified are observed in circulation, repeat testing and evaluation of the animal for hematopoietic neoplasia is indicated.
Reactive vs neoplastic?
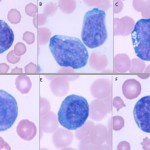
Reactive lymphocytes should be distinguished from neoplastic hematopoietic cells. This is particularly the case when the cells in question are large or “big blue” cells. Refer to the diagnostic algorithm and table in the related links below for help to determine if a large mononuclear cell with blue cytoplasm is a reactive lymphocyte or a neoplastic “blast”.
Related links
- Diagnostic algorithm for distinguishing between reactive and neoplastic large cells (“big blue” cells) in blood.
- Table for guidelines on distinguishing between reactive and neoplastic large cells (“big blue” cells) in blood.
