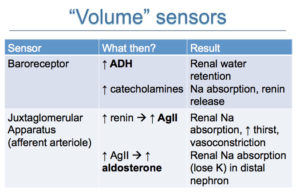
In states of hypovolemia, baroreceptors in the carotid sinus (high pressure) and left atria (low pressure) respond to decreases in pressure caused by decreases in effective circulating volume (hypovolemia) by stimulating ADH release, which causes water without sodium retention in the kidneys. This is accomplished via stimulation (opening) of water channels (aquaporins) in the collecting tubules, which then permit water to move down a concentration gradient into the hypertonic renal medulla (hence you need a hypertonic medulla in order for ADH to conserve water and concentrate urine). Catecholamine release is also stimulated and causes sodium and water absorption in the proximal tubules of the kidney and vasoconstriction as well as stimulation of renin release. Decreased arterial pressure in the afferent arteriole of the glomerulus stimulates the renin-angiotensin-aldosterone system, which causes sodium and water absorption in the distal nephron (under the influence of aldosterone) and proximal tubules (under the influence of angiotensinII) and thirst (water intake without sodium, in response to angiotensinII). Aldosterone simultaneously stimulates K excretion in exchange for sodium and also stimulates hydrogen (acid) excretion by stimulating the H-ATPase. AngiotensinII also stimulates acid excretion via stimulating renal ammoniagenesis in the proximal tubules (NH4Cl loss). These responses to hypovolemia are very effective at restoring blood volume or effective circulating volume, particularly the thirst reflex and aldosterone.