Other hematopoietic-derived leukocytes that are not normally seen in blood include histiocytes (a global term applied to either dendritic cells or macrophages) and mast cells.
Histiocytes
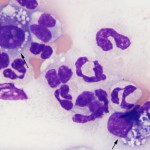
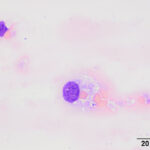
Histiocytes is an umbrella term comprising monocyte-derived macrophages and dendritic cells. All of these cells are derived from a common myeloid progenitor in the bone marrow and are antigen-presenting cells. These cells are not normally in blood, but cells resembling macrophages (eccentric round nuclei, abundant vacuolated cytoplasm, phagocytic activity) can be seen in blood in both reactive and neoplastic conditions. Reactive conditions include inflammation (e.g. pancreatitis in dogs), immune-mediated hemolytic anemia, and infectious organisms (e.g. feline infectious peritonitis [see image to the right and feline blood gallery under the Atlas], systemic mycoses like histoplasmosis and protozoal infections, such as cytauxzoonosis in cats). In some of the mycotic cases, the causative organism may be observed within the cell (and potentially neutrophils as well, since neutrophils can also be phagocytic). In cases of hemolytic anemia, usually with an intravascular component), macrophages may be erythrophagocytic and/or contain hemosiderin in the cytoplasm, obtained from iron within the porphyrin ring of phagocytized hemoglobin. Hemosiderin may also be seen in neutrophils and monocytes (with the cells being called sideroleukocytes) in this setting. In rare cases of dogs with cholestasis, we have seen bile casts within neutrophils and histiocytes (see canine blood gallery under the Atlas). Erythrophagocytic activity by monocytes or macrophages in blood and hemosiderophages (macrophages with hemosiderin in their cytoplasm) can be seen in reptiles secondary to tissue hemorrhage (George et al 2008). Such a mechanism is also conceivably possible in other species although is not recognized as such. Histiocytes or macrophages can also be observed in blood in histiocytic and non-histiocytic neoplasia, such as lymphoma and hemangiosarcoma, in dogs. Large numbers of histiocytes, particularly those with abnormal nuclear features, should raise suspicion for underlying histiocytic sarcoma or dendritic leukemia (a rare variant of leukemia) (Allison et al 2008). Macrophages can also be an artifact of storage (monocytes can become activated over time in vitro and resemble macrophages).
Mast cells
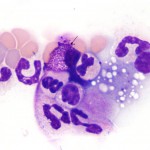
Similar to histiocytes, mast cells are not usually seen in blood of non-diseased animals. Mast cells (mastocythemia) can be seen in the blood of dogs in both reactive (particularly severe inflammation), allergic and neoplastic conditions, including lymphoma and mast cell tumors (McManus 1999). Buffy coat smears to evaluate for the presence of circulating mast cells are frequently requested in dogs with documented mast cell tumors. However, there is no proven correlation between mast cells in blood and metastatic disease. In fact, more mast cells are seen in the blood of dogs with allergies, inflammation and non-mast cell neoplasia than those with mast cell neoplasia. Mast cells are rarely observed in the blood of cats without mast cell tumors, but the presence of low numbers of circulating mast cells in blood (1-2 cells/smear) are not diagnostic for a mast cell tumor in cats either (Piviani et al 2013). High numbers of mast cells are seen in blood of dogs and cats with systemic or visceral mastocytosis (originating in the spleen). When present in low numbers, mast cells are most readily observed at the feathered edge of the blood smear.
