This non-traditional approach to acid-base assessment involves consideration of strong ions and the effects of proteins on acid-base status. The strong ion approach is quite complicated and uses many formulas, which are beyond the scope of this content. However, this approach can be very useful because it is:
- More physiologic than the traditional way of assessing acid-base status and
- Optimal for determining the best treatment for acid-base abnormalities.
Advantages of the strong ion approach for diagnosis of acid-base disturbances are nicely outlined by Constable (2014), who also provides relevant equations, pertinent to cattle.
The main points about the strong ion approach that will be addressed here are general principles, the strong ion difference, and different types of acid-base disturbances identified by this approach. At Cornell University, we use a combination of the classic blood-gas interpretation (pH, bicarbonate and base excess = metabolic, pCO2 = respiratory) and strong ion approach, particularly with respect to strong ions (measured electrolytes and unmeasured, e.g. lactate).
General principles
- Electroneutrality must be maintained.
- Acid-base status is primarily determined by the lungs (which alter pCO2) and kidneys (which alter strong ions).
- There are independent (altered by processes outside the body) and dependent (affected by internal changes or independent variables) variables.
- Independent variables:
- pCO2: Altered by alveolar ventilation. Interpreted as standard approach.
- Strong ions: These are fully dissociated at a normal pH and exert no buffering effect. They include Na+, Cl–, Ca2+, Mg2+, and organic acids, e.g. β-hydroxybutyrate, lactate. Na+ and Cl– concentrations are particularly affected by renal excretion and absorption. The influence of these strong ions on the pH and HCO3– is expressed as the strong ion difference (SID) and BE.
- Nonvolatile weak acids (or Atot): These acids that are not fully dissociated at physiologic pH and include proteins and phosphate.
- Dependent variables: These are interpreted as for the traditional approach.
- HCO3–
- H+
- Independent variables:
Strong ion tests
Strong ion difference (SID)
The strong ion difference is the difference between negatively and positively charged strong ions. Since Na+ and Cl– are the most abundant strong ions, it is relatively simple to calculate the SID(inorganic) from Na+ and Cl–, as follows:
SID(inorganic) = Na+ + H+ = Cl– + OH–,
rearranging this yields:
SID(inorganic) = Na+ – Cl–corr = OH–– H+.
- High SID = alkalosis (increased OH– or decreased H+) and is due to loss of Cl– (metabolic alkalosis) or gain of Na+ (called a contraction alkalosis). Remember, that of these parameters, only Na+ and Cl– are independent.
- Low SID = acidosis (decreased OH– or increased H+) and is due to a gain of Cl– (hyperchloremic metabolic acidosis) or a loss of Na+ (called a dilutional acidosis, although the term “dilutional” acidosis is incorrect per Constable 2014).
Note the SID(inorganic), as calculated above, does not detect unmeasured strong anions (XA‑, e.g. lactate, sulfates) that would cause a titration metabolic acidosis. However, the contribution of these unmeasured strong ions can be taken into account with other formulae, e.g. calculating the unmeasured strong ion concentration [XA–] or the strong ion gap (similar to the AG). Therefore, the SID(inorganic) must be interpreted in conjunction with the AG or [XA–], i.e. a normal SID but a high AG or [XA–] indicates a titration metabolic acidosis.
Weak acids (Atot)
This includes phosphate and proteins, particularly albumin, which are weak anions (or acids). Renal or respiratory compensatory mechanisms do not occur in response to changes in Atot.
- High Atot = hyperphosphatemic acidosis or hyperproteinemic acidosis. An increase in protein, particularly albumin (e.g. dehydration) will result in a mild decrease in pH.
- Low Atot = hypoproteinemic alkalosis. A decrease in albumin will result in an increase in pH.
Unmeasured strong ions [XA–]
Unmeasured strong ions include lactate, ketones (β-hydroxybutyrate, acetoacetate), and sulfates. The presence of these XA– can be evaluated using several formulae, only one of which will be given here. In this formula, [XA–] is estimated by their contribution to the base excess (BE); since XA– are anions, they will cause an acidosis and decrease the BE.
[XA–] = BE – (change in albumin + change in phosphate + change in free water + Cl–corr),
where, change is the difference between the midpoint of the reference interval and the measured concentration of the specific analyte (see Cl–corr previously for an example). The change in free water uses a formula involving sodium concentrations and the normal strong ion difference. Hence, this just adds complexity to the analysis.
- High [XA–] = metabolic acidosis due to an increase in unmeasured strong ions.
Summary of strong ion approach
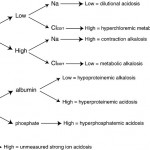
The strong ion approach can identify a metabolic alkalosis and acidosis (see table below) and is superior to the traditional method of assessing acid-base status by inclusion of Atot and free water. Changes in free water alter Na+ and Cl– proportionally, therefore the Cl–corr will be normal, however by decreasing a strong cation (Na+), a gain of free water will cause an acidosis (dilutional) whereas a loss of free water will increase a strong cation (Na+), causing an alkalosis (contraction). In the traditional approach, you may come across the term contraction alkalosis being applied to conditions causing loss of NaCl in excess of water and bicarbonate, such that the extracellular fluid “contracts” around the remaining electrolytes.
| Disturbance | pCO2 | SID | Atot | [XA–] |
| Acidosis | ↑ | ↓ | ↑ | ↑ |
| Alkalosis | ↓ | ↑ | ↓ |
